Pulse Plethysmography: How It Works and Why It Matters
Pulse plethysmography measures blood volume changes with each heartbeat using light, pressure, or impedance. This guide explains the technology, clinical uses, and key measurement methods.
Pulse plethysmography is the measurement of volume changes in tissue or blood vessels that occur with each heartbeat. The term covers a family of related techniques, all of which detect the pulsatile component of blood flow but using different physical principles: light, electrical impedance, air pressure, or mechanical displacement.
The most widely used form today is photoplethysmography (PPG) — the optical method that powers wearable heart rate monitors and clinical pulse oximeters. But the broader family of plethysmographic techniques has a 150-year history in clinical medicine, and several non-optical forms remain in active use for vascular assessment and limb blood flow measurement.
What "Plethysmography" Means
The word comes from the Greek plethysmos (enlargement) and graphein (to record). Plethysmography records enlargement — specifically, the rhythmic expansion and contraction of tissue or blood vessels driven by the cardiac cycle.
In every form of plethysmography, the fundamental principle is the same: blood arriving with a heartbeat increases volume at the measurement site, and that volume change is detected and recorded over time to produce a continuous waveform.
Types of Pulse Plethysmography
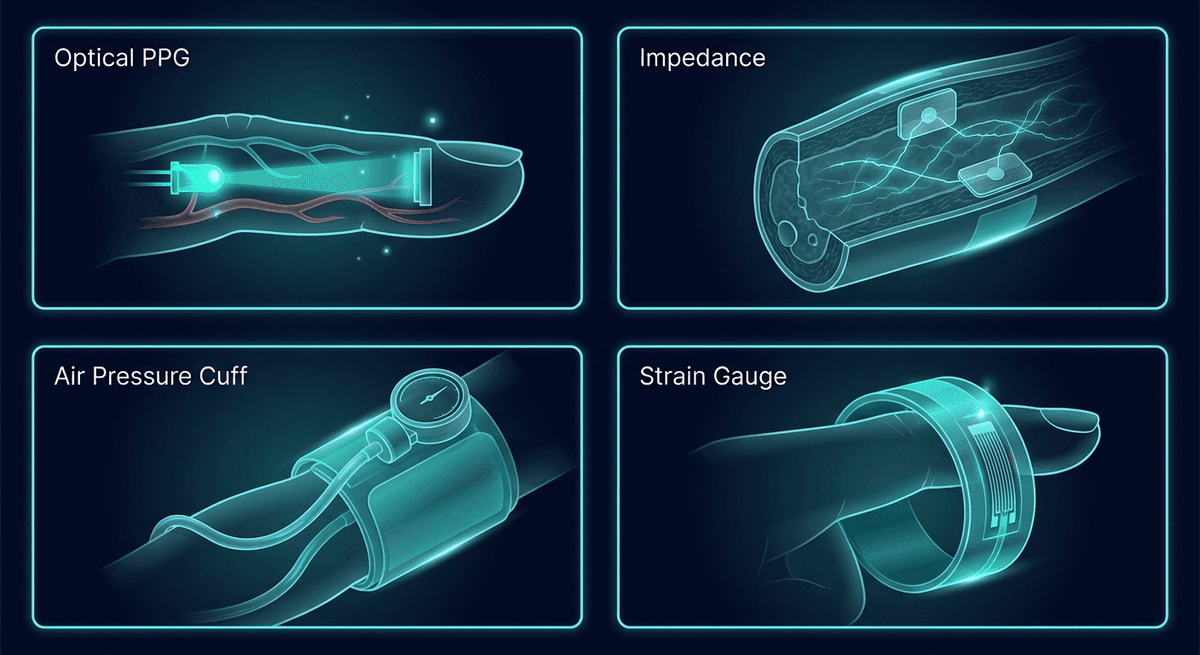
1. Photoplethysmography (PPG) — Optical
The dominant method in modern wearables and clinical monitoring. An LED shines light (typically green, red, or near-infrared) into tissue, and a photodetector measures reflected (or transmitted) light intensity. Blood absorbs more light than surrounding tissue, so increased blood volume with each heartbeat reduces detector output.
PPG is simple, cheap, power-efficient, and can be miniaturized into a chip smaller than a fingernail. It is the basis for heart rate monitoring in virtually all consumer wearables and for SpO₂ monitoring in clinical pulse oximeters. Its primary limitation is sensitivity to motion artifact and optical interference from ambient light.
For complete details, see our PPG sensor technology guide and introduction to PPG signals.
2. Impedance Plethysmography
Uses electrical impedance (resistance to alternating current) to detect blood volume changes. Electrodes placed around a limb or body segment measure how impedance changes as blood volume varies. Blood conducts electricity better than tissue, so impedance decreases when blood volume increases.
Impedance cardiography (ICG) applies this principle to the thorax to non-invasively estimate cardiac output and stroke volume. By analyzing the rate of impedance change (dZ/dt), the timing of aortic valve opening and closing can be identified, allowing stroke volume calculation.
Bioelectrical impedance analysis (BIA) used in smart scales and body composition monitors is related but does not specifically measure cardiac pulsations — it measures whole-body fluid distribution using low-level AC currents.
3. Air/Fluid Plethysmography (Volume Displacement)
The oldest form, dating to early 20th century vascular physiology labs. A limb is sealed in a rigid chamber filled with air or water. Blood flowing into the limb displaces air or fluid, which is detected by a pressure transducer.
Venous occlusion plethysmography (VOP) applies a pressure cuff to briefly block venous outflow while allowing arterial inflow. The rate of limb volume increase during occlusion directly measures arterial blood flow. It remains a research gold standard for measuring limb blood flow and endothelial function (via forearm blood flow responses to vasodilators like acetylcholine).
4. Strain Gauge Plethysmography
Mercury-in-silicone or conductive rubber strain gauges wrap around a limb. As blood pulses through, the limb expands slightly, stretching the gauge and changing its resistance. Often used alongside venous occlusion protocols for research blood flow measurement. More sensitive than air plethysmography for detecting small volume changes.
5. Pulse Volume Recording (PVR)
A variant of air plethysmography using segmental pressure cuffs on the legs. Multiple cuffs at thigh, calf, and ankle levels inflate slightly and then detect pulsatile volume changes. PVR is used in vascular surgery clinics to assess the severity and location of peripheral artery disease (PAD). It complements Doppler ankle-brachial index (ABI) measurements.
Why Pulse Plethysmography Is Clinically Useful
All forms of pulse plethysmography share a key advantage: they are non-invasive and detect functional blood flow rather than just anatomical structure. They answer the question "is blood getting there?" rather than "is the vessel open?"
Peripheral Artery Disease Assessment
Reduced or absent pulses in the legs detected by PPG or PVR can localize occlusive lesions before more invasive imaging. The pattern of waveform loss at successive leg segments helps distinguish aortoiliac disease from femoropopliteal occlusion.
Autonomic Function Testing
PPG waveform amplitude varies with sympathetic tone. The vasoconstrictor response to a deep breath (the PPG vasomotor response) is a reproducible test of sympathetic nervous system function, used in research and clinical autonomic labs.
Endothelial Function
Reactive hyperemia PPG (RH-PPG) measures the increase in PPG signal amplitude in a finger after brief arm ischemia (tourniquet occlusion). The hyperemic response reflects endothelium-dependent vasodilation — a proxy for nitric oxide signaling and endothelial health. Endo-PAT (Itamar Medical) commercialized this approach as a finger-based endothelial function test with FDA clearance.
Vascular Aging
PPG-derived augmentation index and pulse wave velocity surrogates correlate with arterial stiffness measured by tonometry. Population studies have used PPG waveform features to derive vascular age estimates and cardiovascular risk scores. See our PPG vascular age guide.
The Shift to Wearable PPG
Of all the plethysmographic methods, only PPG has successfully made the transition from laboratory instrument to mass-market consumer product. The reasons are practical:
- Miniaturization: A complete PPG front-end (LED + photodiode + AFE chip) fits in a sensor footprint smaller than a thumbnail.
- Power efficiency: Modern PPG sensors operate at under 100 µA average current — compatible with multi-day battery life.
- Cost: Commodity PPG sensor modules cost under $1 at scale.
- No calibration required: Unlike impedance plethysmography, no calibration is needed for heart rate extraction.
The tradeoff is that wrist-based reflective PPG is considerably noisier than finger-based transmission PPG or clinical-grade setups. But algorithms have advanced dramatically — deep learning models can now extract heart rate, HRV, SpO₂, respiratory rate, and even early-stage AF detection from noisy wrist PPG data with clinical-relevant accuracy.
Comparing Plethysmography Techniques
| Method | Signal | Typical Site | Key Application | Limitation |
|---|---|---|---|---|
| Photoplethysmography | Light | Finger, wrist, ear | Wearable monitoring, SpO₂ | Motion artifact |
| Impedance | Electrical | Thorax, limb | Cardiac output, blood flow | Less sensitive to small signals |
| Air/venous occlusion | Pressure | Forearm, calf | Blood flow, endothelial function | Lab-bound, uncomfortable |
| Strain gauge | Mechanical | Finger, limb | Blood flow research | Fragile, lab-bound |
| Pulse volume recording | Pressure | Leg segments | PAD assessment | Low resolution, non-continuous |
Frequently Asked Questions
What is the difference between plethysmography and photoplethysmography? Plethysmography is the general category of techniques that measure blood volume changes with each heartbeat. Photoplethysmography (PPG) is the specific optical method — using light rather than pressure, impedance, or mechanical strain to detect those changes. All PPG is plethysmography, but not all plethysmography is PPG.
Is a pulse oximeter a plethysmograph? Yes. A pulse oximeter contains a PPG sensor (two LEDs at different wavelengths and a photodetector). It uses PPG to detect the pulsatile signal and then calculates SpO₂ from the ratio of pulsatile signals at the two wavelengths. The "pleth" waveform displayed on a pulse oximeter or hospital monitor is the raw PPG waveform.
What does a plethysmograph measure? Directly, it measures volume or volume changes at a tissue site. In practice, a pulse plethysmograph specifically measures the rhythmic volume changes caused by cardiac pulsations. This indirectly encodes heart rate, pulse amplitude (proportional to flow), waveform shape (reflecting vascular properties), and timing (related to blood pressure and conduction velocity).
Is pulse plethysmography painful? No. PPG is completely non-invasive and painless. Venous occlusion plethysmography involves a pressure cuff inflation that causes mild discomfort during occlusion (similar to having blood pressure taken), but it is temporary and well-tolerated in research settings.
Can pulse plethysmography detect peripheral artery disease? It can raise suspicion and localize the level of disease. Reduced or absent pulse waveforms on PVR traces at specific leg segments indicate obstruction at or above that level. However, it is a screening tool — definitive PAD diagnosis typically involves Doppler ultrasound or imaging.
How accurate is wearable PPG heart rate? In resting conditions, ±2–5 bpm versus ECG reference. During moderate exercise, ±5–10 bpm typically. During vigorous exercise with significant motion, accuracy degrades further and varies by algorithm, device, and individual. See our wrist PPG accuracy limitations guide for specifics.
References
-
Allen, J. (2007). Photoplethysmography and its application in clinical physiological measurement. Physiological Measurement, 28(3), R1–R39. https://doi.org/10.1088/0967-3334/28/3/R1
-
Wilkinson, I. B., & Webb, D. J. (2001). Venous occlusion plethysmography in cardiovascular research: methodology and clinical applications. British Journal of Clinical Pharmacology, 52(6), 631–646. https://doi.org/10.1046/j.0306-5251.2001.01495.x
-
Hamburg, N. M., & Benjamin, E. J. (2009). Assessment of endothelial function using digital pulse amplitude tonometry. Trends in Cardiovascular Medicine, 19(1), 6–11. https://doi.org/10.1016/j.tcm.2009.03.001
-
Tamura, T., Maeda, Y., Sekine, M., & Yoshida, M. (2014). Wearable photoplethysmographic sensors—past and present. Electronics, 3(2), 282–302. https://doi.org/10.3390/electronics3020282