PPG Oxygen Desaturation Index in Wearables: How ODI Helps Screen for Nighttime Breathing Problems
PPG oxygen desaturation index in wearables helps summarize repeated overnight drops in SpO2, offering useful screening for sleep-related breathing problems.
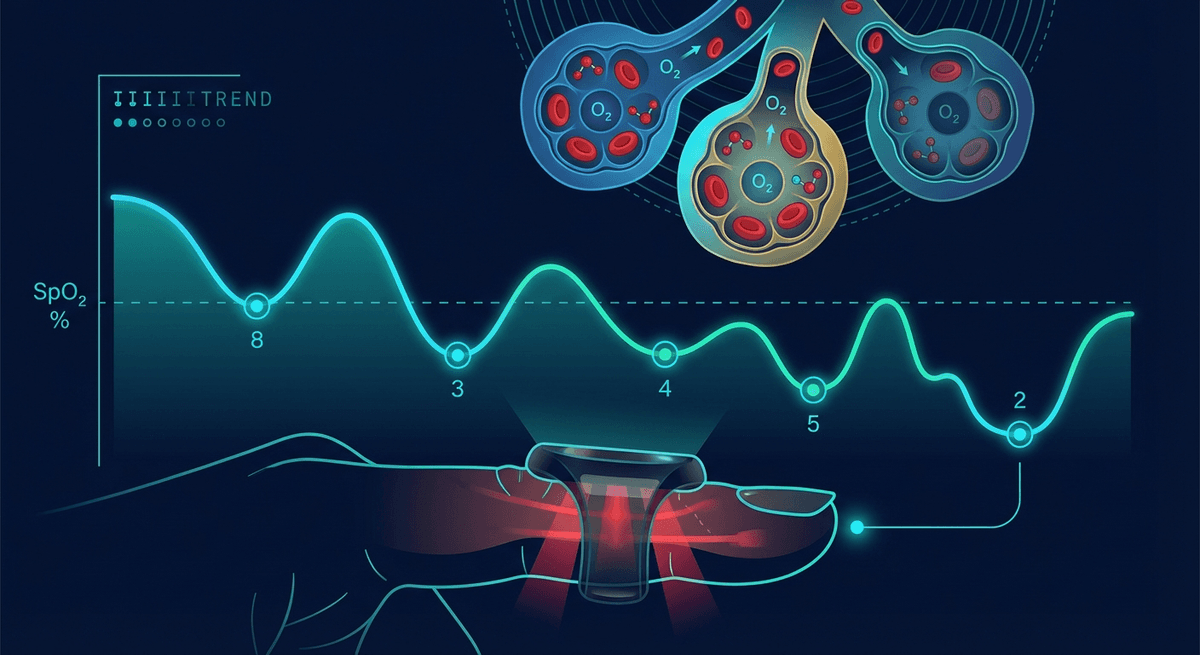
PPG oxygen desaturation index in wearables summarizes how often oxygen saturation drops during sleep, usually expressed as events per hour. It is one of the most practical pulse-oximetry metrics for sleep screening because it compresses a long overnight trace into an interpretable number, but it still reflects oxygen drops rather than the full physiology of sleep apnea.
Definition box: Oxygen desaturation index, or ODI, is the number of desaturation events per hour of sleep or recording time, often defined using a 3% or 4% drop threshold.
This is one of the clearest examples of why wearable data can be useful without being definitive. ODI is simple enough to understand and strong enough to screen, yet limited enough that it should never be mistaken for a complete sleep diagnosis.
Why ODI is useful in wearables
A full overnight SpO2 trace can be messy. ODI turns that into a summary count of events.
That helps with:
- repeated night-to-night comparison
- screening for sleep-disordered breathing
- triage for formal sleep testing
- monitoring changes after treatment or weight loss
For many consumers and even some clinicians, a number like 15 events per hour is easier to grasp than a long waveform.
How does a wearable compute ODI?
The basic process is straightforward:
- collect overnight SpO2 estimates from dual-wavelength PPG
- establish a baseline or rolling reference
- detect drops meeting a preset threshold such as 3% or 4%
- count qualifying events
- divide by hours of valid recording
That sounds simple, but implementation details matter a lot.
Threshold choice
A 3% threshold captures more events but may increase false positives. A 4% threshold is stricter but may miss milder events.
Averaging time
Long smoothing windows reduce noise but can hide short desaturations.
Artifact rejection
Motion, low perfusion, and poor contact can create fake events unless the algorithm excludes bad windows.
ODI versus AHI: why people confuse them
ODI and apnea-hypopnea index are related, but they are not the same thing.
ODI
Counts oxygen drops.
AHI
Counts apneas and hypopneas based on airflow and respiratory physiology.
A patient can have respiratory events that do not cause strong desaturation. Another patient can desaturate for reasons unrelated to classic obstructive apnea. That is why ODI is a useful proxy, not a perfect substitute.
If you want the broader sleep-disordered breathing context, PPG sleep apnea detection and PPG nocturnal hypoxemia monitoring go deeper.
What makes wearable ODI trustworthy or untrustworthy?
Better conditions
- low nighttime motion
- strong perfusion
- stable fit
- finger or well-validated sensor site
- high percentage of usable recording time
Worse conditions
- loose wear
- wrist-only weak signal
- cold extremities
- intermittent data gaps
- smoothing that hides short events
This is why two devices can give different ODI values from the same night.
Who benefits most from wearable ODI?
People with sleep apnea symptoms
Snoring, daytime sleepiness, witnessed apneas, and morning headaches make ODI screening more relevant.
Cardiometabolic risk populations
Patients with hypertension, AF, obesity, and diabetes are common screening candidates.
Follow-up after intervention
ODI trends may improve with CPAP, weight loss, positional therapy, or oral appliance use.
Home monitoring programs
Repeated low-friction ODI estimates can help identify who needs escalation.
What ODI cannot tell you
ODI alone cannot reliably determine:
- obstructive versus central events
- sleep stage-specific burden
- airflow limitation without desaturation
- arousal-only respiratory events
- the full clinical severity of sleep-disordered breathing
That is why wearable ODI should be framed as a screening metric, not the final answer.
Best practical use today
The strongest role for wearable ODI is triage. A consistently elevated ODI across multiple nights, especially in a symptomatic patient, is a strong reason to pursue formal sleep testing. A normal ODI does not completely rule out sleep disorder, but a persistently abnormal ODI is hard to ignore.
FAQ
What is oxygen desaturation index?
Oxygen desaturation index, or ODI, is the number of times per hour that oxygen saturation falls by a defined amount during sleep.
How is ODI different from AHI?
ODI counts oxygen drops, while AHI counts apneas and hypopneas, so the two are related but not interchangeable.
Can a wearable calculate ODI?
Yes. A wearable with overnight SpO2 capability can estimate ODI, though accuracy depends on signal quality, averaging, and device design.
Is ODI enough to diagnose sleep apnea?
No. ODI is a screening metric, not a full diagnosis, because some respiratory events do not cause strong desaturation and other conditions can also lower oxygen.
When is a high ODI concerning?
A repeatedly elevated ODI, especially with snoring, daytime sleepiness, or cardiovascular risk factors, should prompt formal sleep evaluation.
Why ODI is appealing for consumer products
ODI works well in consumer interfaces because it is simple enough to explain and clinically grounded enough to matter. It turns a noisy overnight physiology problem into a rate-based summary that users and clinicians can discuss.
That simplicity is also its weakness. People may assume ODI captures all sleep breathing pathology, when it really captures just one important slice of it.
What makes multi-night ODI more powerful
A single night can be misleading because body position, alcohol, congestion, and sleep stage distribution all change from night to night. A wearable that calculates ODI across many nights provides a more stable screening picture than a one-off estimate.
Frequently Asked Questions
- What is oxygen desaturation index?
- Oxygen desaturation index, or ODI, is the number of times per hour that oxygen saturation falls by a defined amount during sleep.
- How is ODI different from AHI?
- ODI counts oxygen drops, while AHI counts apneas and hypopneas, so the two are related but not interchangeable.
- Can a wearable calculate ODI?
- Yes. A wearable with overnight SpO2 capability can estimate ODI, though accuracy depends on signal quality, averaging, and device design.
- Is ODI enough to diagnose sleep apnea?
- No. ODI is a screening metric, not a full diagnosis, because some respiratory events do not cause strong desaturation and other conditions can also lower oxygen.
- When is a high ODI concerning?
- A repeatedly elevated ODI, especially with snoring, daytime sleepiness, or cardiovascular risk factors, should prompt formal sleep evaluation.