PPG AF Burden Monitoring: What Wearables Can and Cannot Tell You About Atrial Fibrillation Load
PPG AF burden monitoring helps estimate recurring irregular rhythm over time, but wearable burden is still an approximation that needs ECG context.
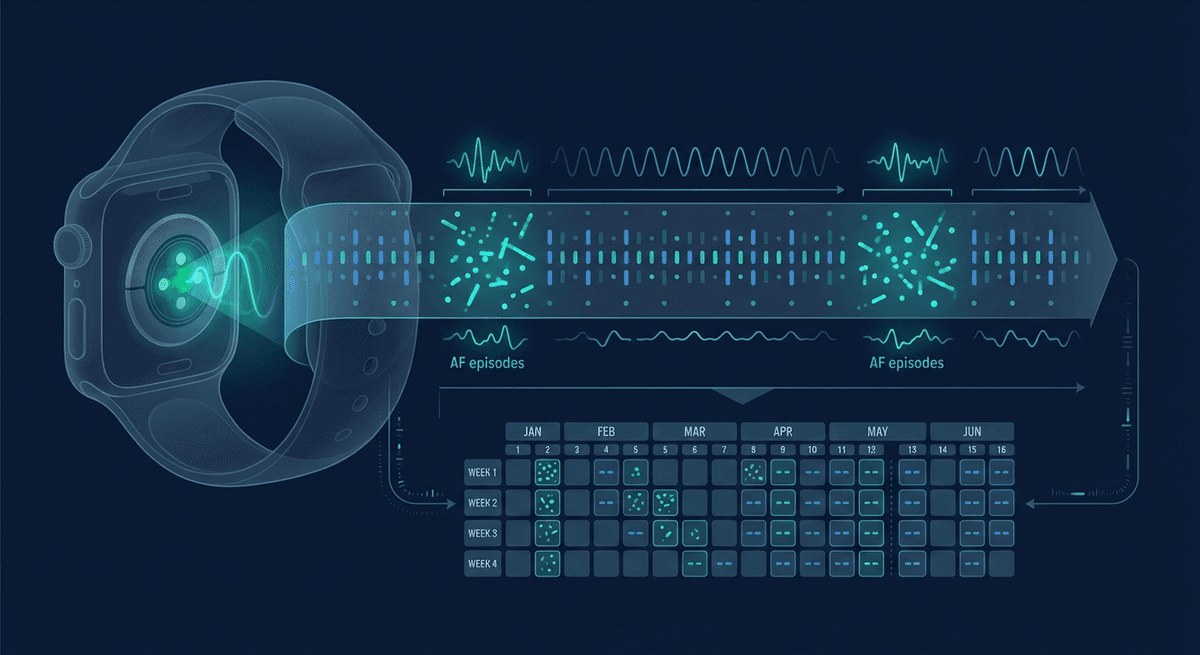
PPG AF burden monitoring uses repeated optical pulse recordings to estimate how much time a person may be spending in atrial fibrillation. That is useful for surveillance and screening, especially across weeks or months, but wearable burden is still an approximation because PPG sees pulse irregularity, not the heart's electrical rhythm directly.
Definition box: AF burden is the amount of atrial fibrillation over a monitoring interval, often expressed as percentage of time in AF or cumulative episode duration.
This distinction matters because many people hear a smartwatch alert and assume it means a clean, exact measure of arrhythmia time. It does not. What a wearable really offers is repeated rhythm suspicion across many everyday moments. That can still be clinically valuable.
What does AF burden mean in practice?
There are two common ways clinicians think about burden.
Episode-based burden
How many AF episodes occurred, and how long did they last?
Time-based burden
What proportion of the total monitored time appears to be AF?
In clinical electrophysiology, the most reliable burden estimates come from ECG patch monitors, implantable loop recorders, pacemakers, or defibrillators with rhythm storage. Wearables sit earlier in that funnel.
Can PPG estimate AF burden at all?
Yes, but with caveats. PPG-based systems can look across repeated time windows, identify irregularly irregular pulse patterns, and summarize how often those windows appear. That creates a burden-like metric.
What makes that possible:
- beat-to-beat interval analysis
- signal quality filtering
- rhythm classification across many segments
- passive data collection over long periods
What limits it:
- PPG does not see P waves or QRS complexes
- frequent ectopy can mimic AF
- motion can create false irregularity
- missed beats change burden estimates
For the broader screening context, PPG atrial fibrillation screening and PPG cardiac monitoring applications are useful companion pieces.
Why clinicians care about burden, not just presence
AF is not all or nothing. A single brief episode and persistent all-day AF are very different clinical states.
Burden can matter for:
- symptom correlation
- recurrence after ablation
- progression from paroxysmal to more sustained AF
- decisions about more intensive monitoring
- understanding whether a notification is a rare event or a recurring pattern
It is important to say this clearly: burden by itself does not determine every treatment decision. Stroke prevention especially depends on broader clinical risk, not just smartwatch numbers.
Where PPG AF burden tracking is most helpful
Longitudinal surveillance
A patient may not wear a patch monitor for months, but they may wear a watch every day. That makes the wearable useful for trend detection.
Post-treatment follow-up
After cardioversion or ablation, recurring irregular rhythm notifications can prompt earlier clinical re-evaluation.
Silent AF discovery
If a person has no symptoms but repeated nighttime irregular rhythm windows, burden-like estimates may reveal that the issue is not isolated.
Trigger identification
Alcohol, sleep deprivation, illness, and endurance exercise can change episode frequency. Consumer wearables are good at showing pattern shifts around those triggers.
Where PPG burden estimates can mislead
This is the part many marketing pages gloss over.
Ectopy inflation
Frequent PACs or PVCs may make the device think AF is present more often than it is.
Missing-data bias
If the wearable excludes noisy periods, the final burden estimate may reflect only cleaner windows, not the whole day.
Sampling gaps
Some devices do not monitor continuously. They sample intermittently or emphasize periods of inactivity. That means burden may be undercounted.
Notification thresholds
Consumer devices often favor specificity. That means they may ignore borderline or short events, again making the burden estimate incomplete.
Why ECG is still the reference
AF diagnosis and precise burden estimation still belong to ECG-based systems because they directly characterize cardiac electrical activity. PPG remains a pulse surrogate.
An ECG can:
- confirm the rhythm mechanism
- separate AF from ectopy or flutter in many cases
- define timing more precisely
- support formal medical decision-making
That is why PPG burden is best used as a trend layer, not as a final clinical endpoint.
Best framing for patients and clinicians
The best question is not, what exact percentage of time was this patient in AF according to a smartwatch? The better question is, does the wearable suggest recurring irregular rhythm often enough to justify further action or closer follow-up?
That framing keeps the technology useful without pretending it is more exact than it is.
FAQ
What is AF burden?
AF burden is the proportion of time or number of episodes during which a patient is in atrial fibrillation over a defined monitoring period.
Can a smartwatch measure AF burden?
A smartwatch can estimate irregular rhythm exposure, but ECG-based systems remain more reliable for true AF burden measurement.
Why does AF burden matter?
AF burden can influence symptom interpretation, monitoring strategy, post-ablation follow-up, and understanding of disease progression.
Can PPG overestimate AF burden?
Yes. Frequent ectopy, poor signal quality, and rhythm classification errors can make wearable AF burden appear higher than it truly is.
When is PPG AF burden tracking most useful?
It is most useful for trend tracking, recurrence surveillance, and identifying people who should receive confirmatory ECG monitoring.
What patients should avoid doing with smartwatch AF burden data
The biggest mistake is changing medication, especially anticoagulation, based on consumer burden estimates alone. Another common mistake is assuming that no alerts means no AF. Sampling gaps and conservative thresholds can miss events.
The right use of the data is discussion, not self-treatment.
Why nighttime burden trends can be especially useful
Nighttime data is often cleaner, and some patients show most of their irregular rhythm burden during sleep or early morning hours. That makes overnight burden trends useful for deciding whether formal extended monitoring is worth ordering.
Frequently Asked Questions
- What is AF burden?
- AF burden is the proportion of time or number of episodes during which a patient is in atrial fibrillation over a defined monitoring period.
- Can a smartwatch measure AF burden?
- A smartwatch can estimate irregular rhythm exposure, but ECG-based systems remain more reliable for true AF burden measurement.
- Why does AF burden matter?
- AF burden can influence symptom interpretation, monitoring strategy, post-ablation follow-up, and understanding of disease progression.
- Can PPG overestimate AF burden?
- Yes. Frequent ectopy, poor signal quality, and rhythm classification errors can make wearable AF burden appear higher than it truly is.
- When is PPG AF burden tracking most useful?
- It is most useful for trend tracking, recurrence surveillance, and identifying people who should receive confirmatory ECG monitoring.