PPG as a Biomarker for Mental Health: HRV, Anxiety, and Depression
How PPG-derived heart rate variability and pulse waveform features relate to anxiety, depression, and mental health: the evidence, limitations, and clinical applications.
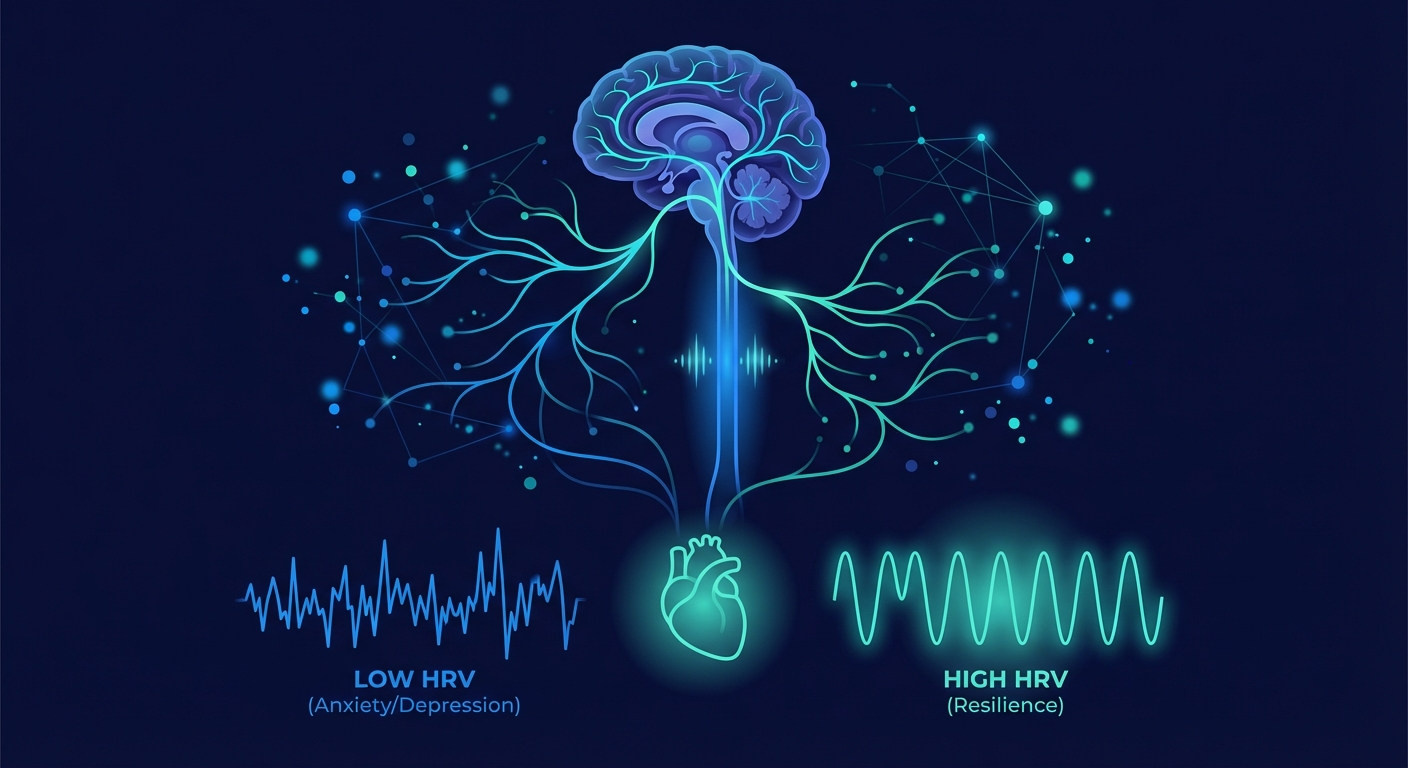
The relationship between the autonomic nervous system and mental health is bidirectional and well-established. Anxiety disorders, depression, and chronic stress all produce measurable changes in heart rate variability, autonomic tone, and vascular reactivity, all of which are accessible via PPG monitoring. Wearable-based mental health monitoring is an active research area with genuine promise and significant limitations.
HRV, derived from either ECG or PPG, has become the primary biomarker connecting autonomic function to mental health. Lower HRV is consistently associated with anxiety disorders, depression, post-traumatic stress disorder, and general psychological distress. The Polyvagal Theory and the neurovisceral integration model provide theoretical frameworks for these associations.
The Autonomic Basis of Mental Health
The vagus nerve, the primary efferent of the parasympathetic nervous system, innervates the heart (among many other organs) and produces the beat-to-beat heart rate deceleration that creates HRV. High vagal tone, reflected in high HRV, is associated with:
- Emotional regulation capacity
- Cognitive flexibility
- Social engagement (a Polyvagal Theory tenet)
- Resilience to stress
Low vagal tone, reflected in low HRV, is associated with:
- Anxiety and rumination
- Difficulty recovering from stress
- Depression
- Cardiovascular risk
This is not merely correlation. Vagal nerve stimulation (implanted or transcutaneous) has demonstrated antidepressant and anxiolytic effects in randomized trials, providing mechanistic support for the HRV-mental health link.
HRV as a Biomarker for Anxiety
Anxiety disorders produce a characteristic pattern of autonomic dysregulation: elevated sympathetic tone, reduced parasympathetic activity, and increased LF/HF ratio in frequency-domain HRV analysis. This produces lower RMSSD, lower pNN50, and reduced high-frequency HRV power.
A meta-analysis by Chalmers et al. (2014, doi:10.1016/j.ijpsycho.2014.01.009) covering 36 studies found that individuals with anxiety disorders had significantly reduced HRV compared to controls, with Cohen's d = -0.46 for SDNN and -0.50 for HF power. The effects were consistent across generalized anxiety disorder, social anxiety disorder, panic disorder, and PTSD.
Specific findings:
Generalized anxiety disorder (GAD): Lower RMSSD at rest, with particular impairment in HRV response to relaxation tasks. GAD patients show difficulty "downshifting" from high to low arousal states, visible in autonomic recovery metrics.
PTSD: Reduced HRV reactivity to trauma-related stimuli, combined with hyperarousal at baseline. A study by Tan et al. (2011, doi:10.1097/PSY.0b013e3182273b24) found that Vietnam veterans with PTSD had RMSSD values approximately 30% lower than veterans without PTSD.
Panic disorder: Acutely elevated heart rate and dramatically reduced HRV during panic attacks, with baseline HRV reductions that persist between episodes.
Social anxiety disorder: Reduced HRV specifically during social interaction tasks, with more preserved resting HRV compared to GAD.
HRV as a Biomarker for Depression
Depression is associated with reduced parasympathetic activity and increased sympathetic tone, producing low HRV. This relationship has clinical implications because low HRV in depression predicts both treatment response and cardiovascular outcomes.
The association between depression and cardiac risk has been recognized since the 1990s. Depression following myocardial infarction triples mortality risk. HRV may be the mechanistic link: depression-associated low HRV indicates the same autonomic dysregulation that predisposes to ventricular arrhythmias.
A meta-analysis by Brunoni et al. (2013, doi:10.1192/bjp.bp.112.117168) found that treatment-resistant depression patients had significantly lower HRV than treatment-responsive patients, and that HRV changes during treatment predicted antidepressant response. This suggests that HRV monitoring during depression treatment could help identify non-responders earlier.
Antidepressant medications affect HRV differently:
- SSRIs generally increase HRV (via serotonergic vagal modulation)
- TCAs reduce HRV (anticholinergic effects)
- SNRIs have variable effects depending on norepinephrine:serotonin ratio
- Exercise therapy consistently increases HRV and has demonstrated antidepressant effects
Wearable PPG for Mental Health Monitoring
Several research groups and commercial products have attempted to translate the HRV-mental health association into practical monitoring:
Daily HRV monitoring apps: Apps like HRV4Training, Elite HRV, and Oura's readiness score track daily HRV from morning resting measurements. In controlled studies, these measurements correlate with subjective mood and stress reports, though the correlation is moderate rather than strong (r = 0.3–0.5 in most studies).
Ecological momentary assessment (EMA) studies: Research using PPG wearables combined with frequent mood questionnaires (EMA) have demonstrated that real-time HRV dips correlate with self-reported anxiety and stress with latencies of 30–90 minutes, enabling some predictive capability.
Machine learning approaches: Several studies have trained ML models on continuous PPG data from wearables to predict self-reported mood and stress scores. A 2020 study by Can et al. (doi:10.3389/fphys.2019.01563) achieved prediction accuracy of 68% for distinguishing high vs. low stress from 5-minute PPG segments, using features including RMSSD, LF/HF ratio, and waveform morphology.
Digital therapeutics: Biofeedback applications that use real-time HRV from PPG to guide paced breathing exercises (typically at 0.1 Hz, which maximizes HRV via resonance frequency breathing) have demonstrated anxiolytic effects in multiple randomized trials. This represents the clearest evidence-based application of PPG in mental health.
The Cardiac Coherence Approach
Cardiac coherence is the state of orderly, high-amplitude HRV oscillations at approximately 0.1 Hz (one cycle every 10 seconds), achieved through paced breathing at that frequency. This state is associated with:
- Enhanced autonomic balance
- Reduced cortisol and perceived stress
- Improved emotional regulation
- Enhanced cognitive performance
Clinical HRV biofeedback at resonance frequency is supported by multiple meta-analyses for anxiety (Lehrer et al., 2020, doi:10.3389/fpsyg.2020.566124) and shows promise for depression augmentation therapy.
Consumer apps and wearables that guide paced breathing using real-time HRV feedback (Inner Balance, Welltory, many smartwatch breathing features) are essentially delivering this intervention, though typically with less clinical structure than research protocols.
Limitations and Cautions
The HRV-mental health relationship, while real, is not simple:
Effect sizes are moderate: The correlation between HRV and anxiety or depression is statistically robust but explains a minority of variance. Many people with severe anxiety have normal HRV; many people with low HRV are not anxious.
Causality is complex: HRV is both affected by and affects mental health. Physical fitness, age, medications, and disease all independently affect HRV. Interpreting a wearable's HRV in mental health terms requires accounting for these confounders.
Individual baselines vary enormously: A 45 ms RMSSD may be high for one person and low for another, depending on age, fitness level, and genetics. Cross-sectional population norms are less informative than individual longitudinal tracking.
Not a diagnostic tool: Low HRV does not diagnose anxiety or depression. Many physiological conditions (cardiovascular disease, diabetes, dehydration) also reduce HRV. Clinical diagnosis of mental health conditions requires formal clinical assessment.
Privacy concerns: Continuous passively collected HRV data that can correlate with mental state raises significant privacy and ethical issues, particularly if collected by commercial entities.
Practical Applications for Clinicians and Patients
Evidence supports the following PPG/HRV applications in mental health contexts:
-
Daily resting HRV as a mood barometer: Morning HRV measurement provides a daily autonomic readiness score. Sustained declining trends may warrant clinical attention or lifestyle intervention.
-
HRV biofeedback for anxiety: Structured paced breathing to resonance frequency with real-time HRV feedback has the strongest evidence base. This can be implemented with consumer PPG devices and validated apps.
-
Treatment response monitoring: Tracking HRV changes during antidepressant or psychotherapy treatment provides an objective physiological correlate. Increasing HRV during SSRI treatment is a positive prognostic indicator.
-
Stress response characterization: During standardized stress challenges (Stroop test, mental arithmetic), HRV reactivity and recovery provide characterize individual autonomic response profiles that inform personalized intervention strategies.
Internal Links
- For HRV measurement methodology and accuracy: PPG HRV Motion Artifacts and Accuracy
- For stress detection methods: PPG Stress Detection Methods
- For cognitive load measurement: PPG Cognitive Load Detection
FAQ
Does low HRV mean I have anxiety? Low HRV is associated with anxiety disorders on a population level, but it is not diagnostic for an individual. Many physiological factors affect HRV, including fitness level, age, medications, and physical health conditions. Low HRV in isolation does not indicate anxiety. If you are concerned about anxiety, clinical assessment is more appropriate than HRV measurement alone.
Can wearable HRV monitoring improve mental health? Wearables that guide HRV biofeedback (paced breathing at resonance frequency, around 6 breaths per minute) have demonstrated anxiolytic effects in clinical studies. Simply monitoring HRV without using it to guide intervention has not been shown to improve mental health outcomes, but may increase self-awareness that facilitates help-seeking.
What is cardiac coherence and how do you achieve it? Cardiac coherence refers to high-amplitude, regular HRV oscillations at approximately 0.1 Hz, achieved by breathing at about 6 breaths per minute. In this state, heart rate accelerates during inhalation and decelerates during exhalation in a regular, large-amplitude pattern. It is associated with reduced stress, improved emotional regulation, and autonomic balance.
How does depression affect heart rate variability? Depression is consistently associated with reduced HRV, reflecting reduced parasympathetic activity. People with depression have lower RMSSD, SDNN, and HF power compared to non-depressed controls. SSRIs generally increase HRV during treatment, and the degree of HRV recovery may predict antidepressant response.
Can I use my smartwatch to track my stress levels? Some smartwatches (Apple Watch, Garmin, Samsung Galaxy Watch) provide stress scores derived from HRV analysis. These scores correlate moderately with self-reported stress in research studies (r = 0.3–0.5). They are useful for identifying personal stress patterns over time but should not be treated as precise measurements of a single stress episode.
What is the neurovisceral integration model of HRV and mental health? The neurovisceral integration model (Thayer and Lane, 2000) proposes that the neural networks regulating cardiac vagal tone are shared with networks regulating emotion, attention, and executive function. High vagal tone therefore reflects both cardiovascular health and neurological capacity for self-regulation. This model explains why HRV correlates with cognitive performance, emotional regulation, and social behavior, not just cardiac health.